A diagnosis of HCM impacts mental as well as physical health. Hear from Lora Peppard, PhD, DNP, PMHNP-BC on interventions that nurses can use to support patients with HCM and lead to improved quality of life, adherence, and long-term health outcomes.
Episode Resources
- HCM & Mental Health
- American Psychiatric Nurses Association connection paradigm
- Spirituality Wellness Assessments
- Mattering Science: Zach Mercurio
- Flourishing Science: Christie Bethel
- PCNA Resources on HCM for Providers and Patients
Thank you to Cytokinetics for the support of this episode.
Lora Peppard podcast episode transcript
I’m Erin Ferranti, board president for PCNA, and I’d like to welcome you to this episode of the Heart to Heart Nurses Podcast. PCNA is the proud home of cardiovascular nurses and one of the leading figures in the fight against cardiovascular disease. We have the resources you need for your day-to-day practice or to follow your passion to new areas of learning and growth.
Until recently, when a patient was diagnosed with HCM, symptom management was the only therapy available. Now, with two approved treatments–mavacamten and aficamten –shared decision-making is more important than ever to ensure that patients, family members and caregivers understand available treatment options
Geralyn Warfield (host): (00:00)
Welcome to our audience for this 3rd of a 3-part series that explores the human side of hypertrophic cardiomyopathy.
Our previous episodes discussed signs and symptoms, guideline-directed disease management, and the role of shared decision-making in patients with HCM.
Today we’re joined by Lora Peppard, and we’re going to be talking a little bit more about the psychological impact of HCM on patients, and how nurses and other healthcare professionals can help patients improve their quality of life and their outcomes.
So that was an awful lot of things that we’re going to cover today, but the first thing that we have is to introduce you to our guest. So, Laura, why don’t you tell us a little bit about yourself?
Lora Peppard: (00:39)
I’m Lora Peppard. I currently run a training and technical assistance division for substance use prevention. It’s a national one for the high-intensity drug trafficking area program. That’s out of the Office of National Drug Control Policy. I’ve been a psychiatric nurse practitioner for 22 years and served on the board of the American Psychiatric Nurses Association. I’ve done a deep dive into connection and what we call health-promoting relationships in the current work that I do.
Geralyn Warfield (01:13)
Well, we are so excited to have you sharing your expertise with our audience today.
And as I mentioned in our introduction, we’re going to be talking about hypertrophic cardiomyopathy, but many of the things that we are going to discuss today are really applicable across the board when it comes to chronic diseases. And I think we all recognize that having a serious chronic disease can be just incredibly stressful for the patient, for the caregiver, for the family, for even the healthcare professionals that are working with that patient.
I’m wondering if you could talk just a little bit more about that stress, that anxiety, and how that really impacts those with chronic diseases.
Lora Peppard: (01:52)
Sure. I mean, all of us go through challenges, and all of us encounter stress in varying degrees in any given day. And stress levels, you know we always say in psychiatry and psychiatric nursing that a mild- to moderate-stress level actually is okay. You want that. It drives us in some way where our body is wanting to alleviate that in some way. And it’s a motivator.
If you think of it on a continuum of, say a scale of one to 10, 10 being complete panic and the worst anxiety that you’ve experienced or stress that you’ve experienced, and 0 being nothing, we usually hover around a 3 to 4 in terms of that’s something that will drive us, and get us going, and moving towards a goal that we have, or a fear that we might want to eliminate, or a relationship we might want to repair.
You know, having a little bit of stress and anxiety is not a bad thing. It’s when it becomes chronic and consistent and elevates beyond that 3 to 4 in any given time. And not to say that you can have stress levels of 8 to 10. And as long as they’re short lived; we’ve all, you take a test, right? Maybe you get a ticket when driving. These are all episodic situations and over time, the stress level goes down pretty quickly. But when we encounter that higher stress level for long periods of time—and stress can be driven by loneliness. It can be driven by pain. It can be driven by fear of the unknown.
And so, when that lingers for long periods of time, then we start to see physiological effects and emotional effects and behavioral effects.
Geralyn Warfield (04:01)
I suspect that all of us have had these periods, as you’ve described, of short-term stress because it’s life. And you’ve also described how this chronic stress can be indicative of some kind of underlying conditions perhaps, or maybe some things that maybe feel out of our control.
So, for example, if somebody has experienced an injury, a loss, and that anxiety stays at an elevated level for a long period of time, we all recognize that there’s some physiological changes that occur in our bodies with the levels of cortisol that increase and inflammation perhaps that occurs, depression and all kinds of things that are associated with whatever the situation might be.
So I’m wondering if you have any suggestions, any clinical pearls, any words of wisdom, that you could provide to healthcare professionals to share with patients, to share with family members, to share with the community that is dealing with these kinds of stresses, and in ways that we can help enable them to decrease that stress or at least address that, those stressors in their lives.
Lora Peppard: (05:09)
I was a practicing provider for 22 years and I really appreciated the large evidence base of strategies that I had at my fingertips, right? And what I think I’ve come to more fully appreciate over the last 3 to 4 years is, beyond those evidence-based strategies that we’re trained in, whether you’re a licensed professional counselor or nurse or medical doctor or medical tech, whatever it is, you have a touch point with these, with humans and those who are suffering, or those who are trying to navigate difficult situations, whatever it is, really.
And what I’ve come to just really appreciate is the power of–beyond these formal evidence-based strategies—the power of the relationship and the power of thinking about their healing through the lens of connection. And it’s not just social connection. I definitely want to talk about that, but it’s also sensory connection and it’s connecting with their selves, right, with their own being. And it’s connecting spiritually.
And with the American Psychiatric Nurses Association, we developed a connection paradigm that kind of represented an organized way of thinking about those four domains. But just off the top of my head, immediately what some of the main points might look like if you’re a provider and you want to engage these various forms of connection to help promote healing and stress management and recovery in a way that can bring peace throughout that recovery.
You can begin by thinking about the senses, right? And really looking at this through the lens of how can I engage and actively invite them into reflection? Upon how can I engage their sight and their hearing and touch, right? Smells to bring not just a sense of relief or calm or decrease anxiety, but to also bring a part of their treatment strategy that they can come to rely upon to consistently bring those factors into the whole journey.
So, an example of this might be, in what ways do smells bring you peace? So, an example is, we’re all familiar with aromatherapy, right? But it could be something different, like the smell of green grass or the smell of frost or the smell of walking through nature, just anything having to do, sometimes that conjures up a belief system of something bigger and it can help them remember that there is something bigger going on for them. There is a purpose, right? They can find meaning within this if they look within, and that then can draw them into a strength that they can find from spiritual connection.
If someone is spiritual and they find strength and hope within their spirituality, then actively engaging them in thinking through that and how they can access it more readily, how they can grow within it to build that strength and build those spiritual muscles, if you will, so that they can more easily access it when they’re in pain, or when they’re feeling isolated, or when they’re too tired to get up, but they really want to engage in life in some way.
So, sensory connection really facilitates connection in all of these other domains like spiritual connection and even connection with self. One thing that I do that I’ve polled a few people and not many people do this but I’m a big smells person and when I wake up in the morning, I ask myself, how do I want to approach today? What am I getting done today? What mood am I looking for today? Because there are a variety of moods. Maybe I’m going to be writing that day and I want to be contemplative and thoughtful. And there are certain smells that will trigger that more easily for me.
Or maybe I want to be at peace and I’m relaxing with my family that day. And so, I’ll engage a different type of perfume or smell. And so, we find across the board that those who are working through chronic stress of any type, that in thinking through even the touch of water, right? And whether that’s cool water, like a cold plunge to kind of get the endorphins going and dopamine and sugar levels balanced, or a warm bath with some soothing music and smells, whatever it is, it’s unique to them. And the key is in asking them.
The key is in leading them through a process of thinking through, how can I engage my senses as part of this treatment strategy? How can I engage my spirituality as part of this treatment strategy? And very importantly, how can I align within myself my approach to this with what I value and what the highest priorities are for me in my life? Is it a high priority for me to remain engaged with my family no matter what?
Is it a high priority for me to rest and not do as much, right? Be able to say no to certain things so that I can build an environment of recovery for myself. So as providers, we have these tools at our hands, and it simply is a conversation and talking with them and thinking deeply with them about that.
Geralyn Warfield (12:10)
Lora, I really appreciate the fact that you have given us a variety of self-care strategies that we can share with our patients in terms of allowing them to recognize where they are in any given moment of any given day and how best to address that. And we’re going to take a quick break and we will be right back.
Geralyn Warfield
We are back with Lora Peppard to speak about the psychosocial aspects of hypertrophic cardiomyopathy and other related diseases when it comes to having a chronic condition and how that affects our patients and how we can help them address these issues in their lives.
You had mentioned something earlier about the relationship that a professional might have with a patient, or provider might have with a patient. And I think sometimes we make an assumption that things are going smoothly if the patient does not bring it up in a clinical visit, for example.
But are there some ways that we could assess more directly at every visit or on a regular basis to make sure that our patients are not feeling overwhelmed, if there are triggers that are occurring for them. Are there any instruments out there that we might use and what might that look like in practice?
Lora Peppard: (13:24)
Sure. Well, the ultimate outcome, right, is their well-being. That’s the outcome. That’s the North Star. We’re always headed there with them, together. And there are some general well-being assessments that can be used clinically. I also think about it this way, though, if you deconstruct that a little bit and you think about these four domains of connection.
There are spirituality assessments that can be given. So, they assess the spiritual wellness. And that’s kind of a neat thing to do for those in which spirituality is the source of strength and hope for them. Sometimes that opens their eyes to habits that maybe have waned, and maybe that’s something like they used to pray every morning and that stabilizes their day for them/ And maybe they’re noticing they’re not doing that anymore because they wake up in pain.
So, other types of assessments might be relational health, social health, and their ability to engage; social connection. We know the science is clear that we need relationships to be well physically and emotionally, mentally right? We need them. and our life is shorter, our odds of survival are significantly decreased when we don’t have social connectedness in our lives.
Asking simple questions around if we break down what a relationship is, around the frequency of social connection, how many times are they able to have a touch point with someone and a meaningful conversation? Because the science is also clear that the more deep and meaningful the relationships are, the better they are in terms of increasing that odds of survival.
So, the frequency, the variety of relationships, how many relationships do they have in their lives? That, that they encounter on a somewhat frequent basis, but what types of relationships are those, right? Family, friends, at the ice cream shop. You may have, maybe they’re frequenting the ice cream shop because the cold ice cream feels good on their throat, or whatever it is, or maybe it just brings them joy, it’s a subtle sense of joy.
So, we encounter people everywhere we go. And the important piece about relational health and thinking about social connection is that you’ve got the frequency, you’ve got the variety, you’ve got the quality, right? The quality of the relationships, and we can intentionally move into higher levels of quality in our relationships.
So, asking them not just about the quality of their existing relationships, but how are they able to engage? To what extent is that satisfactory to them? Or satisfying.
To what extent is it bringing comfort in some way to talk with someone, not just about what they’re experiencing, but just to have a conversation and feel like they matter.
And so, I honestly would recommend an assessment of mattering. If you can do it, they’ve got them out there. This has been an area, the mattering science, has been an area we’ve been diving into.
So, just sticking on the topic of what we can do to screen for opportunities, to enhance their approach, I would think about it through different lenses. And well-being is a nice universal one.
But then, the more specific you can get in the strategies to address those areas for growth. And mattering is a big one, and it leads a little bit into this discussion around isolation, but being able to assess to what extent do they feel valued and add value. And Zach Mercurio’s work in this field is priceless, in my opinion. I think he’s really exposed a lot of what we need to consider.
Here’s another screener. If you want to think about assessing their ability to flourish, there are flourishing screens out there. I’m reminded of the work of Christie Bethell. She’s done a lot of work when it comes to flourishing science, especially for youth, for early childhood and into adolescence.
Believe it or not, every state measures flourishing now, thanks to her work. There’s a flourishing database and an index of sorts where we get graded as a state on how well we’re doing according to the youth in our state and early childhood as well. So positive childhood experiences are kind of attached to that, but flourishing, well-being, social connection.
And then their ability, I would say finally, to what extent are they able to identify what they value in any given day, orchestrate their life around that and operationalize it, align with that in their daily behaviors, in their daily thoughts, in the way that they feel.
So, they’re making a lot of decisions every day, and we are as well as providers working with them. And so, helping them to make that connection between and activate their agency is a big thing, right? Activate their agency to, ‘you know what, I’m feeling out of control in certain areas of my life, but I actually do have control in these areas.’
And leaning into those will help to strengthen their ability to recover and remain at peace. As they, you can be well, even in the context of suffering, you can be well, even in the context of navigating very difficult things. And our science has given us some glimpses into some strategies for that.
Geralyn Warfield (20:25)
So, for these patients with diseases like hypertrophic cardiomyopathy that are progressive, that are challenging, as you’ve described, would you recommend that we take a different lens when we look at measurements such as activities of daily living?
For example, if the grocery store trip or the trip up and down the stairs is starting to become more of an issue, that might be a segue for us to look at some of these other more intangible things that you’ve described, which still are measurable, but people don’t necessarily recognize.
Do you see the connection between what we’re measuring in terms of, they can walk 10 steps today, they could walk 20 steps the last time I saw them, and a conversation about these really important health-related issues such as flourishing?
Lora Peppard: (21:23)
Yeah, you’re making me think about if physically limited and let’s say one of their values is mobility. And being able to get around and that’s a common one, right? Being able to live life to its fullest as we define fullest, right?
And oftentimes chronic disease or anything that limits us in any way will cause us to question what is most important. What is most important to me within this context where I’m not able to achieve what I traditionally have always been able to achieve? How does that influence, then, my mindset and my shift possibly in then what does become important to me.
And oftentimes, that might shift a value, meaning this: If you’re not able to go out and enjoy your friendships in the same way, if you’re not able to share a meal together in the same way or walk that park together or reconnect, taking a step back and looking at what was it that I was getting from that activity? What was it?
Peeling it back—and beyond the exercise or beyond the good food, you may discover that what you were getting is a sense of feeling understood, of feeling truly seen by that person. Feeling some sense of mattering, or love, agape love, this kind of universal love, or even a friendship love.
And it includes with parents, and with other family members, or even it’s just kind words that are offered by a teacher or a provider. And it’s a moment that you have with them.
And if we can step back and ask ourselves, and providers can help anyone, but especially those sitting right in front of them, think through, what is it about those activities that were satisfying to you, that were meaningful to you? And often, we’ll be able to get to the heart of it, or the spirit of it, which is that, ‘You know, I felt better because I felt connected. I felt like I contributed, or I felt like I was worthy, or that I had something to offer, or
that I could overcome something difficult.’
And lifting a little higher than that even, we start tapping into a belief system. And they probably cultivated or built or reinforced something really positive that made you feel good. And you probably didn’t even recognize that they were fostering this healthy, positive belief within you. You just know that you enjoyed that activity or being with that person.
And primarily this relates to relational health, but not always. It could be going for a run. You know what you really enjoyed about that was you were able to clear your head. You were able to experience decreased anxiety, right?
And so, if we can lift higher and look at the belief system and what we hold to be true, and maybe once uncovered then we can think through different strategies to get there that might revolve around us not being able to get out as much, right? But it doesn’t mean we have to be socially disconnected. It doesn’t mean we have to forego the precursor, what drives why we were doing it in the first place.
You know, oftentimes there is another way to cultivate or reinforce that belief that, maybe it’s that, ‘I’m going to get through this.’ Maybe it’s that, ‘this has purpose for me, that I have a reason to be here.
I just put a bumper sticker on my car today, against my husband’s better judgment. He’s like, ‘Lora, you and the bumper stickers,’ but I don’t have any yet. And this one was one that I just felt very strongly about. It says, “the world is better with you in it.”
And we started looking up the roots of that and that came from some early suicide prevention work. And when I think about isolation, it’s isolation from what? What are you feeling isolated from? And let’s start teasing that out, and putting language to it, and putting character to it so that we can uncover what it is that it was bringing in for you, what it is that it was growing or building so that you can possibly look at it from a different angle and apply different strategies.
Geralyn Warfield (27:22)
I think practically for some individuals, one of the ways that we can provide this sense of community for individuals is through patient resource groups. It’s a way for individuals who are facing similar circumstances to have a chance to have a directed kind of conversation with some of these both higher level thinking, but also ‘here’s how I address not being able to go to the grocery store’ kinds of practicality kinds of things—and in many ways addresses the whole person as a result.
And for practitioners that are finding not enough hours in the day to get everything done, I think it’s a nice way for us to be able to support patients with strategies, with connection, with ways to learn about themselves and learn from others and also contribute to others.
And I find that for some patients that are in these groups, it really is a literal lifesaver for them because it may be the only time that they get a chance to connect with other people during the course of their day. It’s kind of like the Meals on Wheels kind of methodology of making sure that somebody has a touch point every single day or several times a week at least. And I think that’s a practical strategy that often works too.
Is there anything else that you would offer to the people that are listening or watching to this particular episode in terms of key takeaways that you would like them to have?
Lora Peppard: (28:53)
If there was one thing that I would leave you with that has really, it has stuck with me ever since we synthesized the science of relationships and how powerful relationships can be, and influential on preventing various mental health outcomes, preventing suicide, preventing substance use, preventing violence, promoting flourishing and just helping people achieve well-being.
It’s the power of our way of being with people.
And even within a 2-minute touch point with someone, you really can make a difference. And we kind of deconstructed way of being, we put a more formal, more organized way of thinking about it when we did our work around what we call health promoting relationships. And I’ll leave you with these 4 things to think about in any given moment with anyone, not just a patient or a client or a friend or a loved one or colleague. They’re all important, you know.
Ask yourself, what belief am I cultivating in this person in this moment? Think about that. Let that rise to the forefront and be a priority for you when you have these encounters with people.
And then beyond that, think about 4 intentional strategies within your way of being that you can employ that the science shows actually helps to cultivate beliefs like I am seen and loved.
- I’m seen. No matter what you tell me, I’m not going to run away. I’m seen and I’m loved.
- I matter.
- I can overcome hard things. I can influence my life and health/
- And I have support. I have support from you.
So those four intentional strategies to cultivate kind of those 5 core beliefs include this:
Number 1: Create the environment for those beliefs to be cultivated. Ask yourself, what physical and emotional atmosphere am I creating in this moment?
Or have I—think about in an office setting, what are people thinking when they first walk in and they see, do they see a messy office? Do they, do they hear music, peaceful music?
Do they smell something specific? Do I give them a hug? Do they feel something? How’s my tone of voice when I greet them? And what norms or standards am I creating within that environment? What can they expect when they’re coming back to see me? So that’s number one, create the environment so that you can cultivate those protective beliefs.
Number 2 is facilitate connection. And think about those, there are 16, what we call facilitators of connection. And these are qualities or attributes like humility, patience, non-judgment, kindness, authenticity. There’s 16 of these within the connection paradigm, health-promoting relationships. But if we can engage these and I’m telling you, it’s hard to authentically, patience is another one, right? Like to authentically engage these and be fully present with them.
Full presence is another one. But to recognize the value in the depths of what true patience looks like.
So, studying them one-on-one is not something that people do often, but I highly recommend it, and bringing that into the approach. So that’s number two. In what way, how am I connecting with this individual? So what environment am I creating? How am I connecting with them? Is it as effective as it can be? Am I bringing my most connected self forward and am I engaging these facilitators to promote connection with them, so that they build trust with me and they feel seen.
Number 3: And then the third one is something we call micro skills. And micro skills are words and actions, sometimes even our thoughts, but primarily words and actions that we can use, like small specific ones, to cultivate those beliefs.
So, a great example of this is to cultivate the belief of ‘I matter.’ So, keep in mind, you’ve already thought about the environment, you’re now fully present with them, and you’re engaging those facilitators of connection. And then to cultivate the belief of I matter, Zach McIreo recommends that we think about a three-part process.
The first is noticing. Am I asking about how things have been? How did the past 24 hours look for you? And do I notice things about them? Do I notice that you’ve come in with a journal that has some really deep thoughts in it and you spent time clearly thinking about this and I’m noticing that and I want to know more about it. I’m curious.
That’s another universal micro skill being not just fully present, but ‘I’m curious.’ You know, you matter to me. I’m curious about what drove some of those thoughts that you have in that journal. So, I’m noticing that and what, courage and vulnerability it took to write down some of those things, right?
And how strong you are to how insightful you are to really be thinking through how this illness is permeating multiple dimensions of your life. You know, that insight is of great value.
And so, then beyond noticing, the second step is affirming the unique strengths and talents that they’re bringing to that moment, to their journey. So, beyond the courage and the insight. ‘I see within the peer support group that you’re attending every week. You sharing your experience with journaling is making a difference. It’s making a difference in others. I notice how they’re responding to you and how they’re asking you questions. Can you see that the, the impact that you’re having by sharing your journey and your experience?’
So, noticing, affirming, kind of these unique strengths that they’re bringing forward, and the impact that it’s having.
Number 4: And then the final step is needing. So, what he means by that is,
within your words and your actions, sharing with them how you rely upon them, how you need them, how you rely upon them as someone who is taking control and responsibility for their journey.
You’re relying on them, let’s say in this case, “You really are fully committed to this treatment plan and that really helps me as your provider to walk with you through this, because I’m relying on you too.”
Maybe it’s a medication, or maybe it’s a certain exercise that you’ve asked them to do, or there are certain things they can be doing at home. And “how wonderful it is that you are committed to this and you’re doing this and it’s helping. And it helps me then explore complementary options. It helps me to hear from you what’s working and what’s not. So, thank you for giving it your all and for fully investing in your treatment because this matters to me as much as it does to you. And, we’re partners in this together.”
And so, these types of micro skills, noticing, affirming, needing, expressing need, these are micro skills through our words and our actions. when actions might look something like you’re leaning in. And you’re fully present in that conversation with them. And you’re not distracted by that phone that’s going off or the beeper or the Apple watch or the other people that might be coming in and out of the room. They know that you’re fully there with them.
Number 5: And then the final intentional strategy and the way of being right. And this is actually a pretty good one. I hadn’t fully connected it until we started talking through this. But once you have that trusting relationship with them, you’ve created the environment, you’ve facilitated connection, you’ve engaged your micro skills, right? It’s all in an effort to cultivate these protective beliefs that we know will help them propel towards well-being.
You can leverage that, and you can facilitate skill development within them that can also equip them to cultivate those beliefs. And these are things like maybe you teach them how to grow gratitude. Maybe you take 4 or 5 minutes, not even it doesn’t even take that long for grow gratitude, but you lead them through an exercise. Maybe you teach them an exercise on self-compassion.
Maybe you go through hope mapping, and you go through an exercise of cultivating hope through goals, pathways, and agency. They are much more likely to receive the coaching from you to receive that skill development from you. If you’ve done those other three things in your way of being.
And so, in sum, creating the environment, facilitating connection, engaging those micro skills through words and actions, and developing skills within the person that you’re sitting in front of. Or maybe it’s over the screen and you can do all of these things through multiple methodologies, but that’s a four-part way of being intentional, way of being, that the science shows can help send people much closer towards wellbeing.
And it’s something that I just recently looked up the origin of the word intention, and it struck me. It’s Latin. The Latin word is intention and it means stretching with purpose, right? Stretching and purpose. And you’ve put together stretching with purpose.
So, intention as a provider, if you move into your moments with those with
any chronic condition and you say, “I’m going to stretch with purpose today.” And the purpose is to promote their wellbeing and to promote their flourishing. And I had these four strategies that I can engage to do that. That’s what I hope everyone will take away from this podcast.
And together, we can change culture and healthcare. We can create a culture of wellbeing within our healthcare system.
Geralyn Warfield (host): (41:51)
Lora Peppard, thank you so very much for being with us today and for sharing your strategies for helping make the world a better place for our patients, for ourselves, and for everyone that we encounter. This, again, is a 3rd of a 3-part mini-series on the topic of hypertrophic cardiomyopathy. Other episodes will include information and resources for health care professionals and also the perspective of patients. So, we look forward to you sharing those nuggets with us on those other episodes.
Some of the resources that Laura shared with us, we will be making sure that we put those in the show notes so that you have those accessible to you to use in your clinical practice or your daily efforts.
I would like to thank you again, Lora, for being with us today.
I’d also like to thank our supporter, Cytokinetics, for this particular podcast episode mini-series, and we’re really grateful to all of our listeners.
This is your host, Geralyn Warfield, and we will see you next time.
Thank you for listening to Heart to Heart Nurses. Visit PCNA.net for clinical resources, continuing education, and much more.
Topics
- Cardiomyopathy
Published on
March 3, 2026
Listen on:

PhD, DNP, PMHNP-BC
Related Resources
Patient Education Handouts
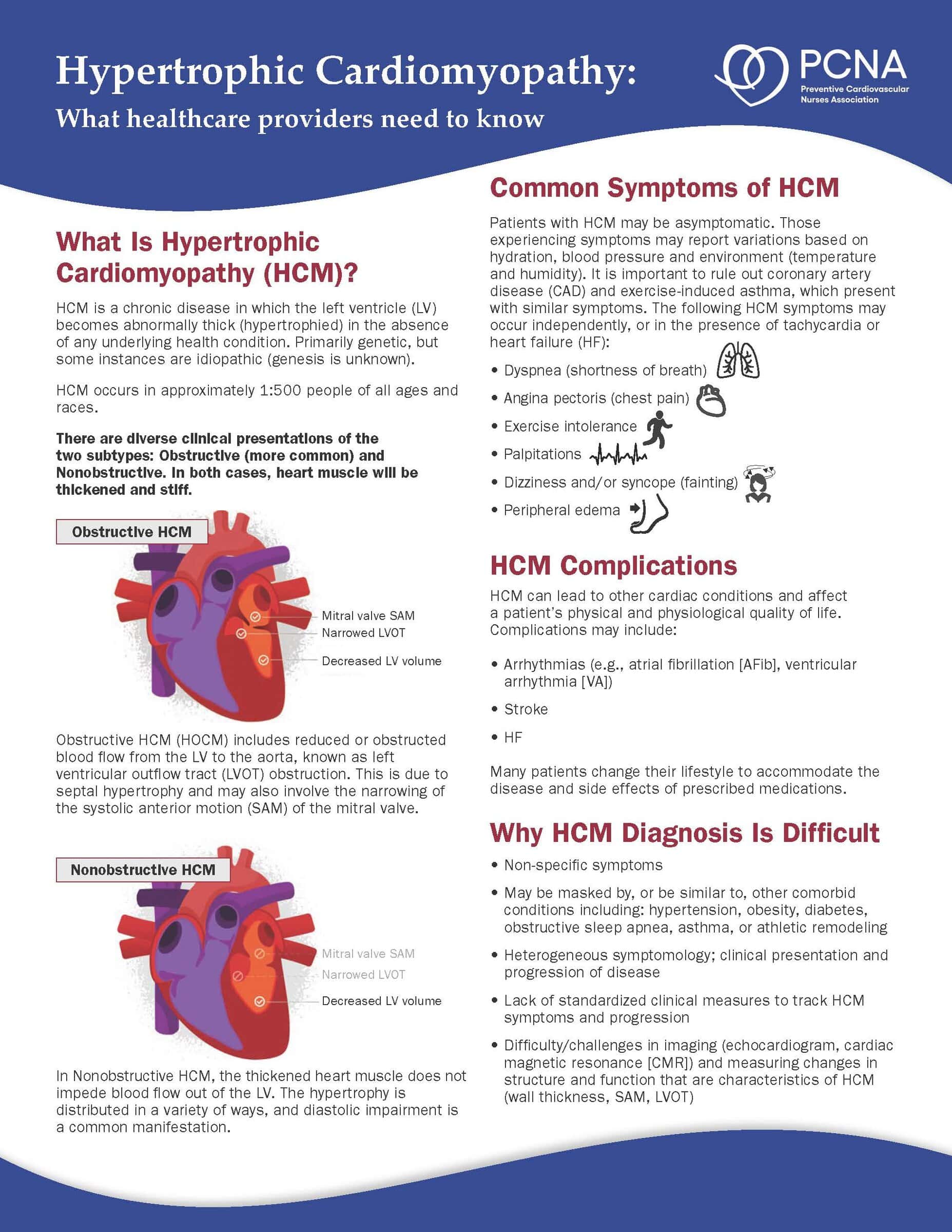
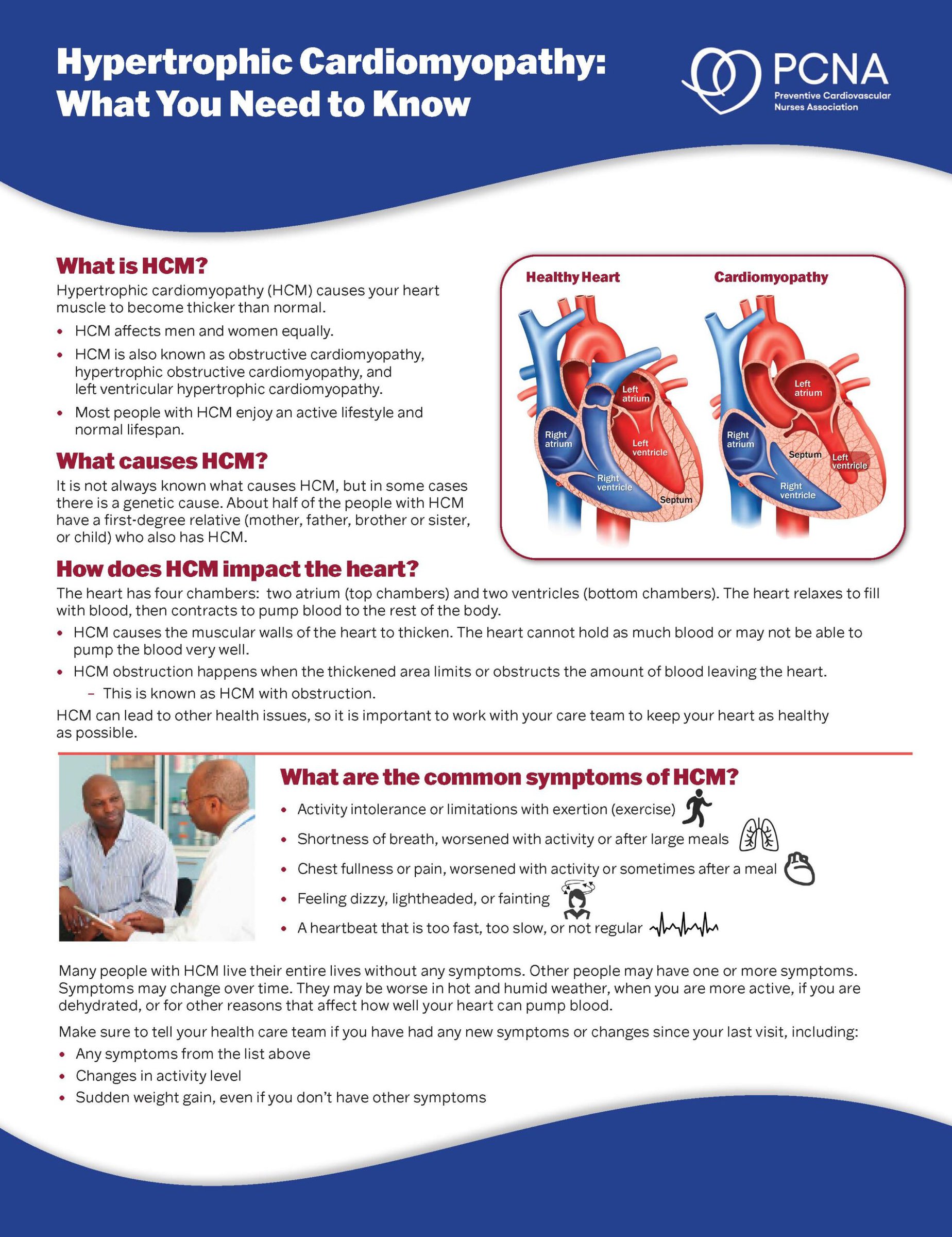
Hypertrophic Cardiomyopathy: What You Need to Know Fact Sheet
October 01, 2025

Patient Education Handouts
Hypertrophic Cardiomyopathy: Is Your Heart Holding You Back? Poster
September 08, 2025






