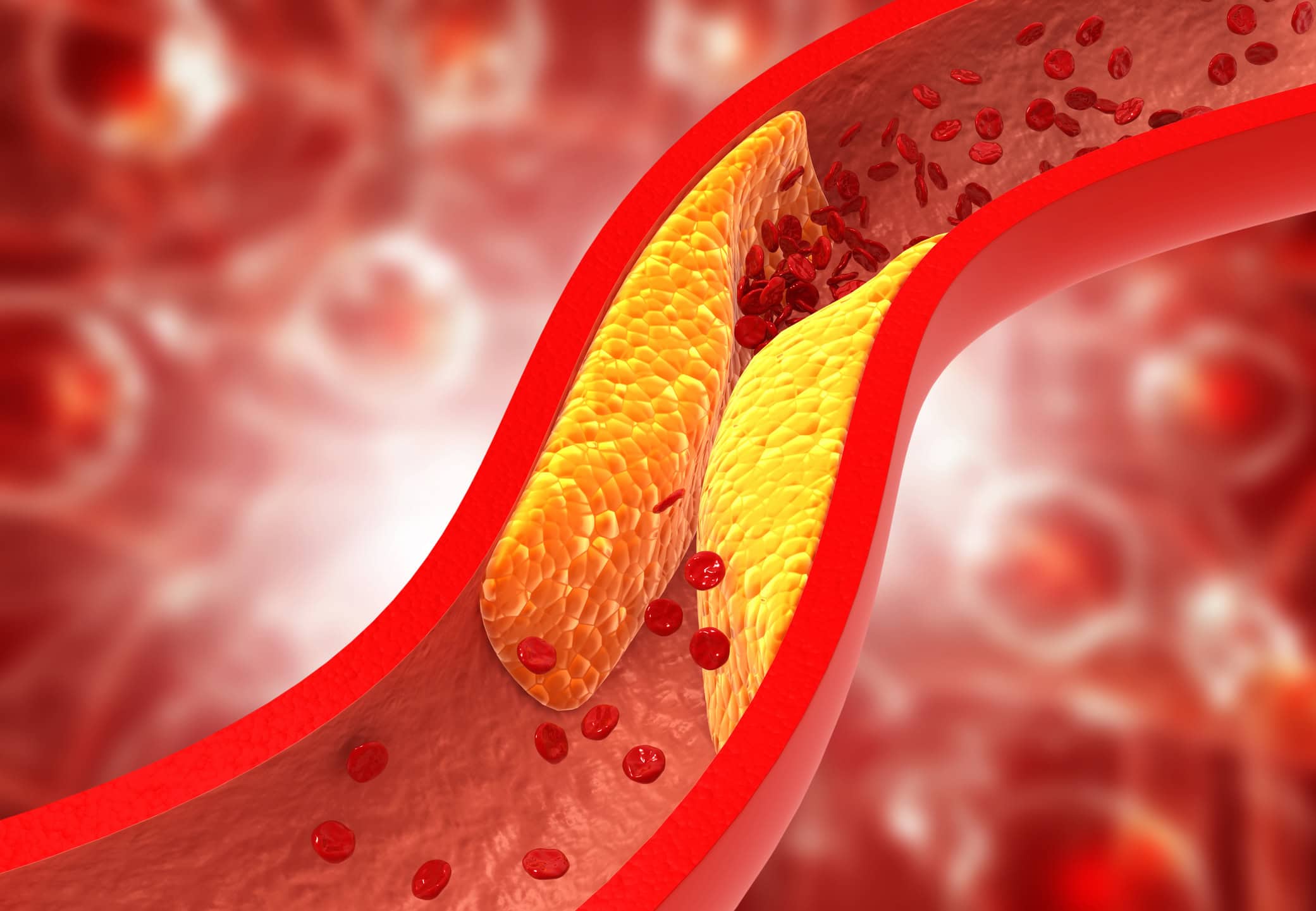
For patients with coronary artery disease, outcomes are improved with early detection, risk stratification, and individualized care. Artificial intelligence (AI) advances are reshaping how the disease is assessed and diagnosed, with enhanced accuracy and efficiency supporting clinical decision-making in ever-expanding ways.
Coronary Artery Disease: Not All the Same
Coronary artery disease (CAD) is the most common type of heart disease1 and is the leading cause of death in adults across the globe.2 In the US, it affects about 5% of the population ages 20 and older, and causes about 40% of cardiovascular-related deaths2 —more than 371,000 in 2022.3
CAD diagnosis typically occurs when a patient presents with chest pain and then undergoes a series of assessments and tests, such as family history, electrocardiography, stress testing, and echocardiography. The goal has traditionally been to identify the amount of arterial blockage that is impairing or restricting blood flow so that appropriate treatments can be employed.
It is important to note that not all heart attacks are caused by severe blockages; non-obstructive coronary artery disease (NOCA) is defined by blockages of <50%. Microvascular dysfunction and coronary spasms also occur, and endothelial dysfunction is often present.
Both obstructive and nonobstructive CAD can lead to heart attack and stroke.
Plaque Volume and Risk
A more complete picture of a patient’s cardiovascular health and risk is possible when healthcare professionals expand their assessments beyond the percentage of arterial blockage. Information about the total amount of plaque, also known as total plaque volume or TPV, is an important factor in clinical decision-making.
A recent retrospective analysis of nearly 8,000 patients identified that the volume of plaque is an independent predictor of long-term cardiovascular events. Patients with the highest total plaque volume experienced more than 5x the risk of major cardiovascular events compared with patients in the lowest stage.4
And there is a long-term risk associated with a higher total plaque volume. Over a median of 3.3 years of follow-up, higher total plaque volume was independently associated with significantly increased rates of cardiovascular death and myocardial infarction.4 Armed with information about plaque volume, healthcare professionals can work with patients in a shared decision-making capacity to identify and implement treatment options for improved health.
Personalized Coronary Artery Disease Prevention Through Coronary Plaque Assessment
It is now possible to provide preventive, personalized cardiac care for coronary artery disease, leading to improved patient outcomes, even when there is no significant arterial blockage. What types of tests are necessary to get the information needed?
- Utilizing an iodine-containing contrast material and CT scanning, a non-invasive Coronary Computed Tomography Angiography (CCTA) allows for the examination of coronary arteries and whether they are narrowed by plaque build-up or artery stenosis.
- Fractional Flow Reserve from CT analysis (FFR-CT) may be added to a CCTA to offer a more precise evaluation of the severity of coronary artery disease. FFR-CTs compare the blood flow on both sides of a blockage to help determine the severity of the narrowing in the artery. Data shows that FFR-CT helps improve decision-making, predict future cardiovascular events, and save costs.4,5
- Artificial intelligence (AI) can aid even further in differentiating potential risk, moving beyond just how much an artery is blocked to measuring the total amount and type of plaque, and whether or not plaque is actually restricting blood flow. This offers a more comprehensive diagnostic output than traditional scans alone.
All of this additional data provides healthcare professionals with a more complete picture of risk and allows for earlier and more personalized interventions. In December 2025, both the American Heart Association and the American College of Cardiology7 released scientific statements about the use of AI-supported techniques in quantitative coronary plaque analysis (QCPA) for risk stratification.
5 Key Takeaways
Coronary artery disease diagnosis and treatment continue to be a challenge for healthcare professionals. The use of AI-enhanced diagnostic tools is assisting in improved detection and risk stratification, leading to individualized care and improved patient outcomes.
- Reducing the rate and impact of coronary artery disease improves quality of life for individuals, reduces morbidity and mortality, and leads to cost savings for care.
- While quantifying arterial blockages is an important step in the identification of coronary artery disease, and informs treatment for obstructive coronary artery disease, even individuals with non-obstructive coronary artery disease are at increased risk of heart attack and stroke.
- Acquiring other noninvasive data, such as the total amount and type of plaque, and whether the plaque is interfering with blood flow, can improve treatment decision-making.
- With access to improved imaging that identifies both the burden of plaque and the impact on blood flow, healthcare professionals can tailor treatment before a cardiac event occurs.
- AI-derived biomarkers and predictive models support personalized risk assessment, assisting nurses and other healthcare professionals in educating patients about their individual risk profiles and collaboratively developing tailored lifestyle and medical interventions.
References
- Centers for Disease Control and Prevention. About Coronary Artery Disease (CAD). May 15, 2024. Accessed January 28, 2026.
- Martin SS, Aday AW, Almarzooq ZI, et al; American Heart Association Council on Epidemiology and Prevention Statistics Committee and Stroke Statistics Subcommittee. 2024 Heart disease and stroke statistics: a report of US and global data from the American Heart Association [published correction appears in Circulation. 2025;151:e1095]. Circulation. 2024;149:e347–e913. doi: 10.1161/CIR.0000000000001209
- Centers for Disease Control and Prevention. Heart Disease Facts. Oct. 24, 2024. Accessed February 9, 2026.
- Fairbairn TA, Mullen L, Nicol E, et al. Implementation of a national AI technology program on cardiovascular outcomes and the health system. Nature Medicine. 2025. 31:1903-1910.
- Bell J. Prognostic value of coronary computed tomography angiography-derived fractional flow reserve (FFR-CT) from a large nationwide cohort. Advances in Science in cardiac computed tomography Session at EACVI. Vienna Austria.
- Slipczuk L, Blankstein R, Bucciarelli-Ducci C, et al. Evaluation and Medical Management of Nonobstructive Coronary Artery Disease in Patients With Chest Pain: A Scientific Statement From the American Heart Association. Circulation. 2025;152(23). doi: 10.1161/CIR.0000000000001394
- Chandrashekhar Y, Blankstein R, Shaw LJ, et al.; for the ACC Quantitative Coronary Plaque Analysis Symposium Collaborators. Quantitative coronary plaque analysis in clinical practice: 2025 ACC scientific statement: a report of the American College of Cardiology. JACC Cardiovasc Imaging. 2025. Accessed January 15, 2026.
Published on
February 26, 2026
Related Resources
Sorry, we couldn't find any resources.